Back pain is not a requirement for having a baby, yet so many expectant mothers treat it like one. You shift your weight, you wince when you stand up from the couch, and you wonder if those aching hips are just part of the deal. They aren’t. Prenatal massage is a specialized form of therapeutic bodywork designed specifically for pregnant women to relieve physical discomfort and reduce stress hormones. It is not simply a regular Swedish massage with a pillow under your belly. It requires specific positioning, modified pressure techniques, and a deep understanding of how pregnancy changes your body’s mechanics.
If you are navigating the physical demands of carrying a child, understanding what this therapy can-and cannot-do for you is crucial. This guide breaks down the safety protocols, the physiological benefits, and exactly what you should look for in a practitioner to ensure a safe and restorative experience.
The Physiology of Pregnancy and Why Your Body Hurts
To understand why standard massage often fails during pregnancy, you have to look at the hormone relaxin. Relaxin is a hormone produced during pregnancy that softens ligaments and loosens joints to prepare the pelvis for childbirth. While this is biologically necessary for delivery, it makes your entire skeletal structure less stable. Your center of gravity shifts forward as your uterus grows, forcing your lower back into an exaggerated curve (lordosis). This puts immense strain on your lumbar spine and glutes.
Furthermore, blood volume increases by up to 50% during pregnancy. This extra fluid can lead to swelling (edema) in the legs and feet. A regular massage might not address this fluid retention effectively, or worse, could aggravate it if the therapist doesn't know how to work with lymphatic drainage safely. Prenatal massage focuses on these specific structural changes. It targets the quadratus lumborum muscles in the lower back, which bear the brunt of the shifting weight, and uses gentle effleurage strokes to help move excess fluid without stressing the kidneys.
- Ligament Laxity: Joints are looser, requiring gentler stretching and stabilization.
- Center of Gravity Shift: Causes chronic lower back and pelvic girdle pain.
- Increased Blood Volume: Leads to edema, requiring careful fluid management techniques.
- Hormonal Sensitivity: Skin becomes more sensitive; oils must be non-comedogenic and safe.
Safety First: Trimesters and Contraindications
Safety is the single most important factor in prenatal care. The general rule of thumb among obstetricians and massage therapists is to avoid massage during the first trimester unless you have a provider who specializes exclusively in high-risk pregnancies. The risk of miscarriage is highest in the first 12 weeks, and while massage does not cause miscarriage, the uncertainty makes many providers hesitant.
Once you enter the second trimester (weeks 13-27), you are generally in the "sweet spot" for prenatal massage. Nausea has usually subsided, your energy levels may be higher, and the risk of preterm labor is low. The third trimester (weeks 28-40) is also safe, but comfort becomes a bigger challenge due to the size of the belly. You may need shorter sessions or more frequent adjustments during the session.
| Trimester | Safety Status | Key Considerations |
|---|---|---|
| First (Weeks 1-12) | Avoid or Consult Doctor | High risk period; nausea may make lying down difficult. |
| Second (Weeks 13-27) | Safe and Recommended | Best time for full-body relaxation; back pain begins. |
| Third (Weeks 28-40) | Safe with Modifications | Comfort is key; focus on short sessions and leg/back relief. |
There are specific contraindications where massage should be avoided entirely. If you have placenta previa, preeclampsia, severe varicose veins, or a history of preterm labor, you must get explicit clearance from your obstetrician. Additionally, certain pressure points, particularly around the ankles, wrists, and sacrum, are traditionally avoided in Chinese medicine because they are believed to stimulate uterine contractions. A qualified therapist will know these zones instinctively.
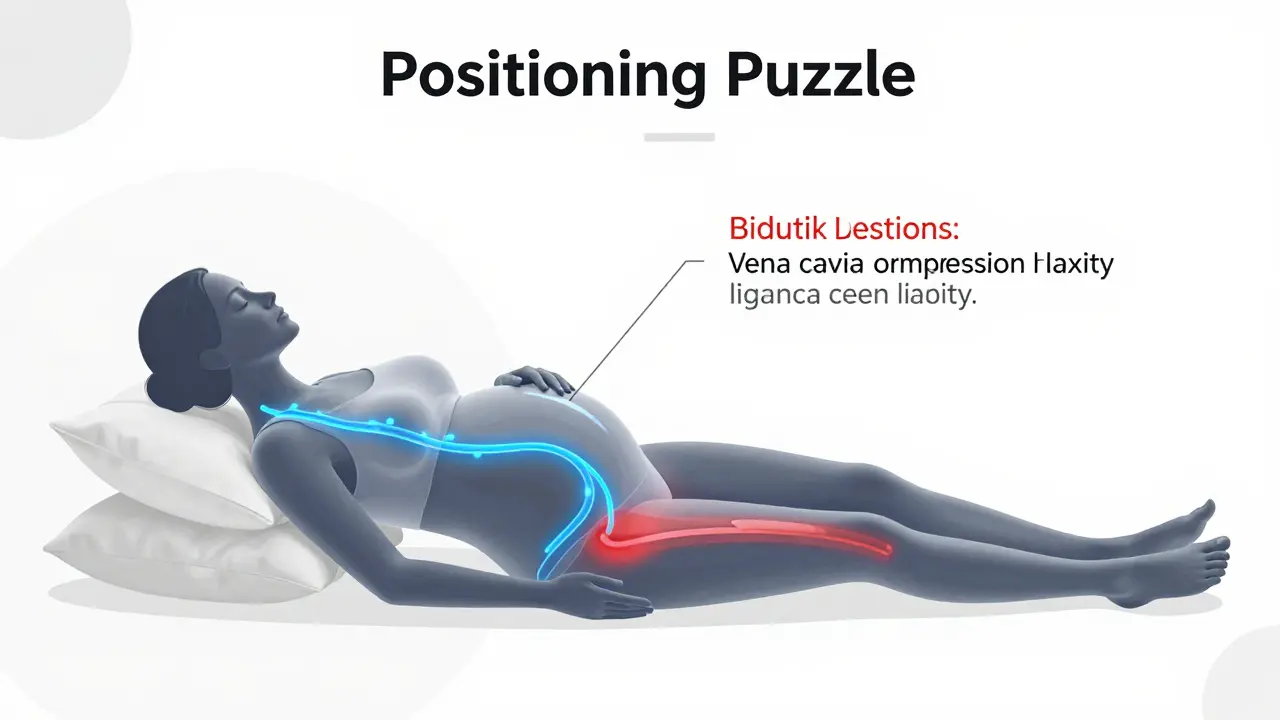
The Positioning Puzzle: Side-Lying vs. Prone
The biggest myth in prenatal massage is that you can lie on your stomach. You cannot. Lying prone (on your stomach) after the first few months compresses the vena cava, the large vein that carries blood from the lower body to the heart. This compression can reduce blood flow to the baby and cause dizziness or fainting in the mother.
The gold standard is the side-lying position. Side-lying involves positioning the client on their left or right side with strategic support under the head, between the knees, and under the abdomen to maintain neutral spinal alignment. This position keeps blood flowing freely to the uterus and prevents strain on your lower back.
A skilled therapist will use a combination of pillows, bolsters, and sometimes a specialized pregnancy massage table with a cutout for the belly. However, even with a cutout, side-lying is preferred for later stages. The therapist will place a pillow between your knees to keep your hips aligned, preventing the top hip from sliding forward. Another pillow goes under your chest to prevent your shoulders from rolling forward. This setup allows them to access your back, hamstrings, and calves without compromising your comfort or safety.
Benefits Beyond Relaxation
We often think of massage as just "feeling good," but prenatal massage offers measurable physiological benefits. Research published in the Journal of Obstetrics and Gynecology has shown that regular prenatal massage can significantly reduce anxiety and depression symptoms during pregnancy. It lowers cortisol (the stress hormone) and increases serotonin and dopamine levels.
Physically, the benefits are immediate and tangible:
- Pain Reduction: Significant decrease in lower back pain, sciatica, and neck pain.
- Swelling Management: Gentle lymphatic drainage reduces edema in the hands and feet.
- Nerve Compression Relief: Helps alleviate carpal tunnel syndrome, which affects up to 60% of pregnant women due to fluid retention.
- Better Sleep: Reducing physical tension helps improve sleep quality, which is notoriously disrupted during pregnancy.
- Fetal Heart Rate Stability: Some studies suggest that maternal relaxation leads to more stable fetal heart rates.
It is not a cure-all, but it is a powerful tool for managing the physical toll of gestation. If you suffer from morning sickness, the aroma of essential oils used in massage might actually trigger nausea. In that case, ask for a fragrance-free session.
Finding a Certified Prenatal Specialist
Not every massage therapist is trained to work with pregnant clients. General massage training covers basic anatomy, but it does not cover the complex biomechanics of pregnancy. You need someone who has completed specific continuing education in prenatal care.
Look for certifications from recognized bodies such as the National Certification Council for Therapeutic Massage and Bodywork (NCCBTMB) or similar local governing bodies in your region. Ask direct questions:
- "How many hours of prenatal-specific training have you completed?"
- "What is your protocol for handling high-risk pregnancies?"
- "Do you require a doctor's note for my current stage of pregnancy?"
A good therapist will ask about your health history before you even touch the table. They will want to know your due date, any complications, and your current medications. If a therapist seems rushed or dismissive of these questions, find someone else. Your safety depends on their expertise.
What to Expect During Your First Session
Your first prenatal massage will likely feel different from any other massage you’ve had. The pace is slower. The pressure is lighter. The therapist will check in with you frequently to ensure you are comfortable. You might feel a bit awkward getting into the side-lying position at first, but the therapist will guide you through it.
Expect them to focus heavily on your legs and feet. These areas carry the most weight and fluid. They may use gentle pumping motions to encourage circulation. On your back, they will work around the sacrum and lumbar area, avoiding deep tissue work directly on the spine. They might also spend time on your neck and shoulders, where tension accumulates from looking down at your growing belly.
After the session, drink plenty of water. Hydration helps flush out metabolic waste released from the muscles and supports your increased blood volume. You might feel relaxed, but also slightly tired. Plan to rest for the rest of the day if possible.
Is prenatal massage safe during the first trimester?
Most experts recommend avoiding massage during the first trimester (weeks 1-12) due to the higher risk of miscarriage and potential nausea. However, if you have a specialist who works with high-risk pregnancies and your doctor approves, it may be possible. Always consult your healthcare provider first.
Can I lie on my stomach during a prenatal massage?
No, lying on your stomach is unsafe after the first few weeks of pregnancy. It can compress the vena cava, reducing blood flow to the baby and causing dizziness. The side-lying position with proper pillow support is the safest and most effective method.
How often should I get a prenatal massage?
For maintenance and general comfort, once a month is sufficient. If you are experiencing significant pain, swelling, or stress, weekly or bi-weekly sessions may be recommended. Listen to your body and adjust frequency based on your needs and budget.
Are there any pressure points I should avoid?
Yes, certain pressure points near the ankles, wrists, and sacrum are believed to stimulate uterine contractions. A certified prenatal therapist will know these points and avoid them. Never attempt deep pressure on these areas yourself.
Does insurance cover prenatal massage?
Coverage varies widely. Some insurance plans cover massage if it is prescribed by a doctor for a specific medical condition like chronic back pain or sciatica. Others consider it purely cosmetic or wellness-related. Check with your provider and ask if the therapist can provide a superbill for reimbursement.
